28 year old female with no PMHx presented to the emergency department at 2 AM with right sided neck pain, dysarthria, nausea and vomiting 30 minutes after popping her neck at a nightclub. Through her garbled speech, she reports sudden onset of diffuse right sided weakness, blurry vision in right eye, photophobia and phonophobia. Stated that she regularly pops her neck due to soreness but has never had anything this before. She endorsed a week of flu like symptoms a week prior which resolved on its own. She has been seen in this ED 7 years prior for right sided neck pain and was diagnosed with torticollis and was lost to follow up. She denied any drug use, alcohol use, or any cigarette use. Through a friend used for collateral, the patient was discovered to have a history of cocaine use but denies any knowledge of use tonight. On arrival, the patient was slurring her words, had an unsteady gait, and was endorsing right sided neck pain and right sided weakness.
Physical exam:
BP 132/86 HR 92 Temp 97.6 F RR 14 SpO2 96% GCS 15
Significant findings: Patient alert and oriented x 3, pupils are 2 mm bilaterally and reactive, noted to have blurry vision in right eye, visual fields 20/20 on left, 20/100 on right, right sided facial droop, 4/5 strength in both right upper and lower extremities, 5/5 strength in left upper and lower extremities, dysarthria is present with slurred speech, no word finding difficulties. Muscular tenderness to the neck present on right lateral neck with associated decreased ROM, did not tolerate brudzinski’s and Kernig’s signs, no obvious tenderness or deformity felt midline. No carotid or vertebral bruits.
DDx: Vascular dissection, stroke/TIA including cerebral/cervical arterial vasospasm, arterial occlusion, toxidrome, horners syndrome, electrolyte derangement
Clinical Course
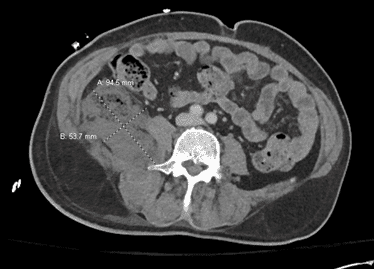
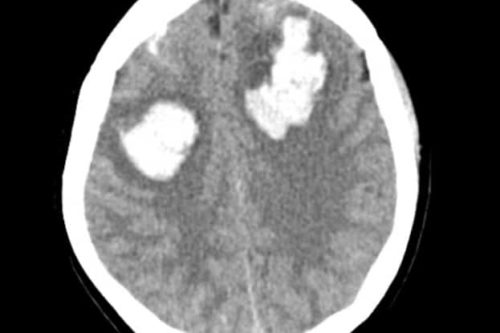
Workup was pursued with CT non-contrast which was negative, CTA head and neck was also curiously negative for any acute abnormalities, incidentally noted dominant left vertebral artery with poorly opacified right vertebral artery was seen, however this was deemed non-occlusive by radiology and secondary to congenital hypoplasia. No findings of dissection or occlusion of any vascular structures.
CTA images:
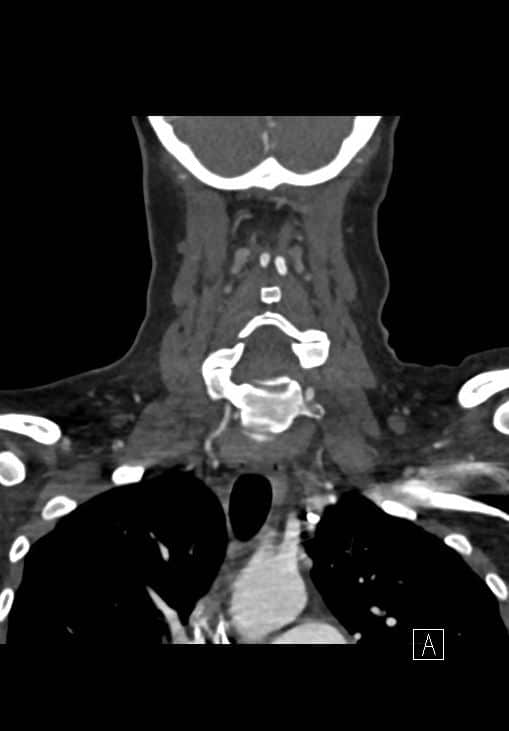

UDS was positive for cocaine, Leukocytosis was noted to 15k otherwise all other labs were unremarkable. Patient was started on empiric antibiotics, antivirals and steroids for concerns for an infectious encephalitis and/or meningitis, Acyclovir, Ampicillin, Vancomycin, and Decadron IV.
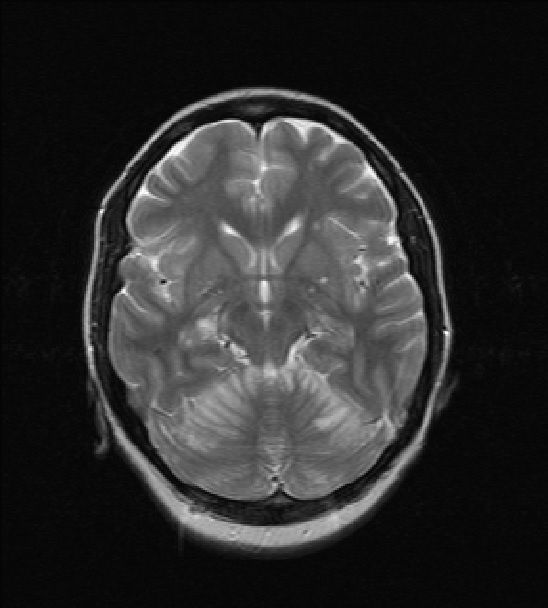
MRI brain revealed nonspecific abnormal edema in superior left and right cerebellar hemispheres favored to represent infectious or inflammatory rhombencephalitis. Additionally small foci of signal abnormality in the periventricular white matter and right thalamus was seen which is usually attributed to microvascular ischemia, thought to be unlikely in her age range and more likely secondary to a vasculitis, demyelinating disease, or atypical infection. MRI cervical spine was unremarkable.
MRI images:

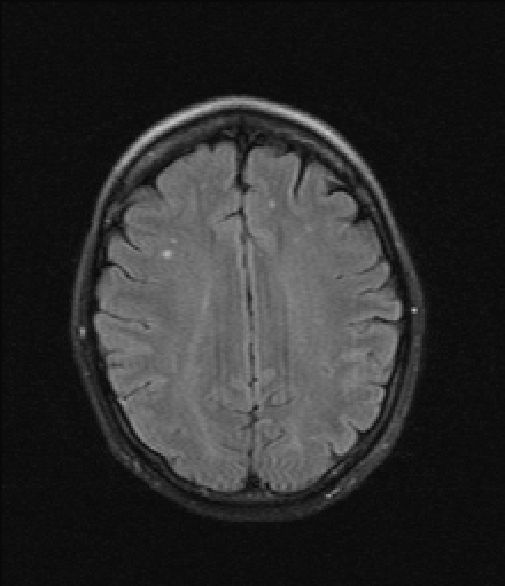
Fluoroscopy-guided LP was subsequently performed and CSF analysis resulted within normal limits, infectious encephalitis/meningitis panel negative. No Ig monoclonal bands or other findings to suggest MS or NMOSD. Over the course of the stay, the patient’s weakness improved and the patient was able to ambulate but minor dysarthria remained. Patient was discharged with PO steroids while awaiting results for a paraneoplastic panel, west nile, lyme disease of her CSF.
Patient returned to the hospital 2 weeks later with AMS as chief complaint, reported GCS 3 and tolerated placement of nasal trumpet without apparent reaction prior to hospital arrival. Patient was hemodynamically stable on arrival and maintaining airway, not requiring NPPV or intubation with SPO2 99% on RA with GCS 3-4. Pt had spontaneous resolution of symptoms with later noted GCS 15 and back to neurologic baseline (no lateralizing deficits but residual dysarthria) while in the ED 2 hours later. Patient then endorsed similar right sided neck pain. Patient was readmitted and had a repeat MRI as well as a repeat lumbar puncture. Results were unchanged from previous, continuing to demonstrate bilateral abnormal signal in superior cerebellar hemispheres and scattered foci.
MRI images from return visit:
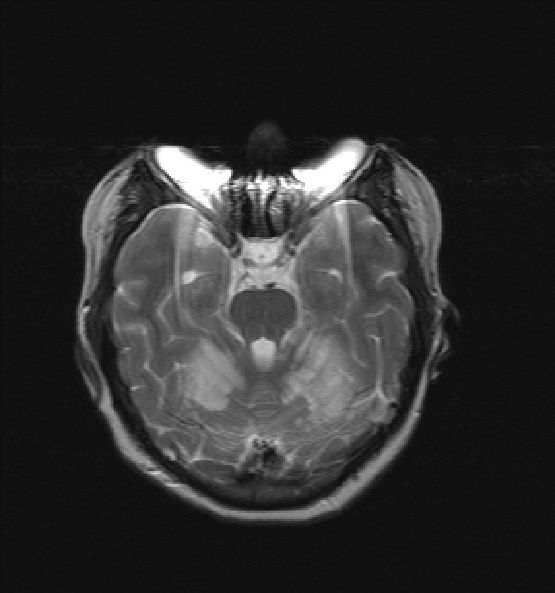
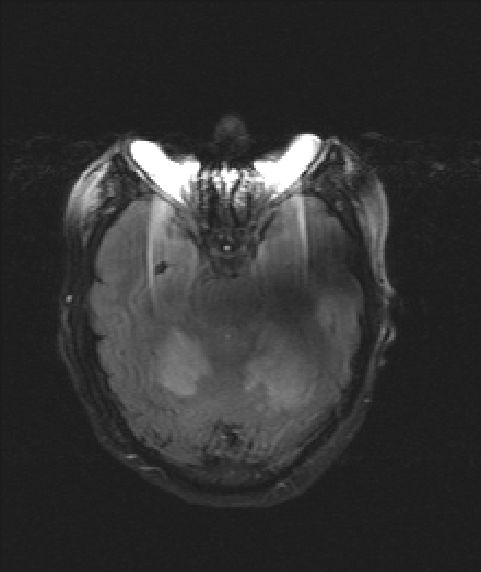
The patient denied any further cocaine use. Paraneoplastic panel returned negative, as well as other autoimmune labs. Patient clinical picture was favored to represent Posterior Reversible Encephalopathy Syndrome (PRES) secondary to cocaine use and the patient was encouraged to follow up with neurology.
Case discussion
At first glance, a presentation of a young patient from a club with slurred speech and altered mental status after self “popping” their neck seems to suggest vascular dissection or toxidrome, possible stroke or vasospasm especially in the case of noted cocaine use. An anticipated relatively straightforward workup and diagnoses. In this case, things were not as they seemed and estimated anchoring bias seemed to be present. The patient had appropriate admission and escalation of imaging when the workup results were not as anticipated eventually leading to a comprehensive diagnosis.
Posterior reversible encephalopathy syndrome (PRES) is characterized by symptoms including headache, seizures, altered consciousness, other neurological deficits and visual disturbances (6). This condition has been known by various names previously (reversible posterior leukoencephalopathy syndrome, reversible posterior cerebral edema syndrome and reversible occipital parietal encephalopathy). The term PRES has been used based on the similarity in the appearance on imaging, the common location of the parietal–occipital lobe, cerebellar or ‘posterior’ location of the lesions. The exact pathophysiological mechanism of PRES is still unclear, but suspected secondary to either cerebral vasoconstriction causing subsequent infarcts in the brain or failure of cerebral autoregulation leading to vasogenic edema. Delayed diagnosis and treatment may lead to mortality or irreversible neurological deficits.
Treatment is typically directed at the underlying cause of the encephalopathy. In hypertension associated or drug-induced PRES, treatment includes withdrawal of offending agent, immediate control of blood pressure, anti-convulsive therapy and temporary renal replacement therapy (hemodialysis/peritoneal dialysis) if required in secondary renal failure. In Systemic lupus erythematosus-related PRES, aggressive treatment with corticosteroids and cyclophosphamide is effective. Corticosteroids may improve vasogenic edema, but there is no substantial evidence for usage in PRES. (8)
Studies on diagnostic error in the emergency department have shown error rates ranging from 1-12%, with flaws in medical decision making suspected to be present in 95% of cases (1). Focusing on cognitive errors can help improve patient care both in the immediate and long term, centering on understanding underlying biases and their consequences on a physician’s actions. There are two broad categories of cognitive errors leading to both improper testing and missed diagnoses; faulty assessment of the disease likelihood and failure to consider relevant alternative diagnoses (2). Contributing to these two broad categories are availability error, affective error, and anchoring error. By using this case as an example, this discussion will focus on a brief review of three of the most common errors identified in the emergency department, and a brief way to combat each.
Availability error is a mental shortcut relying on immediate recent examples which come to a given person’s mind when evaluating a patient. The underlying mental mechanism operates on the belief that if something can be recalled it must be important, heavily basing opinions towards recent or memorable cases instead of the evidence present at hand. This bias can be bidirectional, with positive availability error resulting in overestimation of a disease, which leads to unnecessary testing and expense to the patient, sometimes at the detriment of missing the proper diagnostic test (3). Alternatively, in junior residents the negative effect can occur due to lack of experience leading to underestimation of a disease prevalence resulting in failure to order the proper test (3). In this case, lack of exposure to PRES could lead a junior resident to conclude the patient was likely intoxicated, with failure to order diagnostic labs and imaging at the detriment to the patient. Combating this error centers around systemic thinking, engaging in deliberative reflective decision making and recognizing when decision making is reflexive.
Affective error is when personal feelings about a patient, whether positive or negative, affect medical decision making. Avoiding unpleasant but necessary testing due to sympathy for a patient or not pursuing a standard examination in an unsympathetic patient can quickly lead to medical error and mistakes. In this case, feelings towards an altered patient presenting from a club late at night can lead to premature diagnostic closure and disregard of the clear neurologic deficits, potentially missing the true diagnosis. Acknowledging emotions and avoiding making decisions when viscerally aroused can be difficult but vital in preventing this type of error.
Anchoring error is when a person clings to an initial impression based on limited information, the anchor, despite contradictory evidence accumulating. Oftentimes this conflicting evidence is regarded as anomalies which can be discarded instead of recognizing the need to continue to seek the true diagnosis. In this case, an example would be continued suspicion of alcohol intoxication even with a normal alcohol level. In a similar vein, confirmation bias can lead to ignoring information challenging a diagnosis, leading to premature closure. Anchoring has been shown to occur when under pressure to make a decision quickly, which is very common in the emergency department. To prevent this from occurring, explicitly considering clinical information along with actively seeking information to refute the current provisional diagnosis has been shown to be effective.
Combatting these and other types of cognitive errors have been extensively studied with no clear system shown to be universally effective. Some studies have shown even just an awareness of these cognitive traps leads to improvement and recognition when a physician is falling into one (4). Stopping and creating a cognitive stop point when making a differential diagnosis and attempting to consider alternatives can help to prevent premature closure and diagnostic momentum. This act forces a physician to move from rapid pattern recognition to the less error prone act of deliberation. Addressing systemic issues has also shown benefit, centering on minimizing interruptions and addressing fatigue. When a patient presents with a clear most likely diagnosis, taking a minute to address biases, preconceptions, and cognitive pitfalls can help prevent a serious adverse outcome (5). Overall in this case, PRES was initially very low/absent on the differential diagnosis, but as more pieces came together and with further elucidating of the clinical history, the correct diagnosis was achieved and the patient was able to recover.
References:
- Croskerry P. The importance of cognitive errors in diagnosis and strategies to minimize them. Acad Med. 2003;78:775–80.
- Norman GR, Monteiro SD, Sherbino J, et al. The causes of errors in clinical reasoning: cognitive biases, knowledge deficits, and dual process thinking. Acad Med. 2017;92(1):23–30.
- Hartigan S, Brooks M, Hartley S, Miller RE, Santen SA, Hemphill RR. Review of the Basics of Cognitive Error in Emergency Medicine: Still No Easy Answers. West J Emerg Med. 2020 Nov 2;21(6):125-131. doi: 10.5811/westjem.2020.7.47832. PMID: 33207157; PMCID: PMC7673867.
- Royce CS, Hayes MM, Schwartzstein RM. Teaching Critical Thinking: A Case for Instruction in Cognitive Biases to Reduce Diagnostic Errors and Improve Patient Safety. Acad Med. 2019 Feb;94(2):187-194. doi: 10.1097/ACM.0000000000002518. PMID: 30398993.
- Monteiro SD, Sherbino J, Patel A, et al. Reflecting on diagnostic errors: taking a second look is not enough. J Gen Intern Med. 2015;30(9):1270–4
- McKinney AM, Short J, Truwit CL, McKinney ZJ, Kozak OS, SantaCruz KS, et al. . Posterior reversible encephalopathy syndrome: incidence of atypical regions of involvement and imaging findings. Am J Roentgenol 2007;189:904–12. [PubMed] [Google Scholar]
- Bartynski WS, Boardman JF. Distinct imaging patterns and lesion distribution in posterior reversible encephalopathy syndrome. Am J Neuroradiol 2007;28:1320–7. [PMC free article] [PubMed] [Google Scholar]
- Wada KI, Kano M, Machida Y, Hattori N, Miwa H. Posterior reversible encephalopathy syndrome induced after blood transfusion for severe anemia. Case Rep Clin Med 2013;2:332. [Google Scholar]