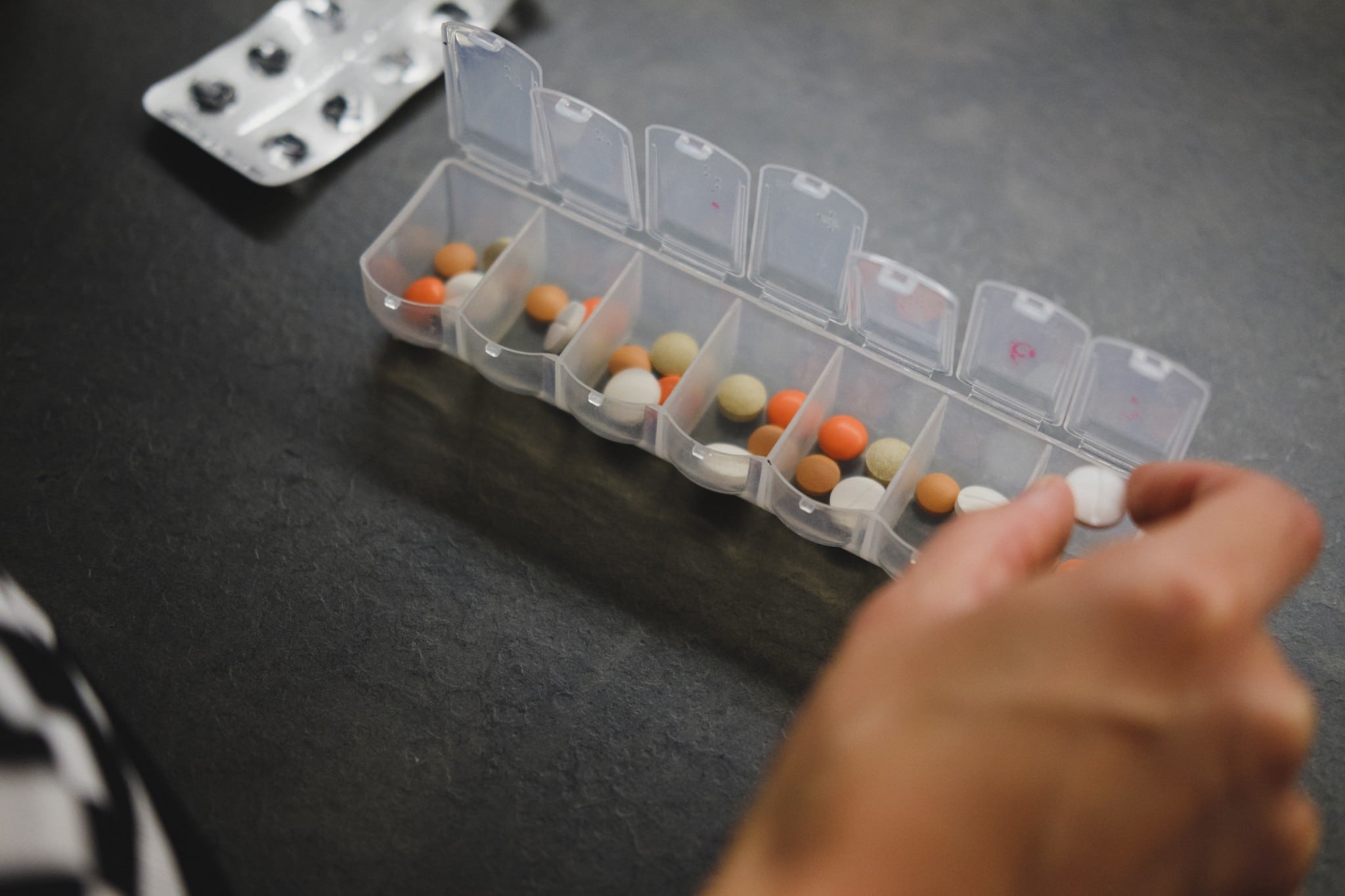
Adverse drug events (ADE) frequently occur among patients with multimorbidity, particularly in elderly patient populations. Though a computer alert clinical decision supporting system (CDSS) has been advocated to prevent injuries from ADE since the 1990s, its optimal outcomes were less reported until the recent emergence of the medication risk score (MRS).1 We read with great interest the study by Ratigan et al., who reported higher MRS associated with higher patient mortality.2
MRS as one of the CDSS’s to improve patient safety and avoid ADE has been reported in recent years.3-5 Such benefits stem from reducing health care utilization (e.g., Emergency Department visits, hospital admissions) to lowering overall health care cost (e.g., reducing an average of over US$1,000 with the decrease of MRS).3 At present, with Ratigan et al.’s findings, these benefits could be expanded to reduce patient all-cause mortality.2 Particularly given that current data points towards most ADE’s being predictable and preventable.1 We expect to see more benefits once MRS-CDSS can be completely aligned with the electronic health record (EHR) system for medicine reconciliations, especially among patients with multimorbidity. Patients with multimorbidity often have polypharmacy, thus avoiding ADE becomes challenging among pharmacists and physicians in these situations. A recent study reported the benefit of pharmacists using an MRS-CDSS, with pharmacists displaying an increased amount of relevant clinical recommendations after participating in a medication therapy management program.4 Additionally, though the mechanism(s) of medications for coronavirus treatment are still not fully understood, a recent simulation-based strategy to assess the risk of ADE for drugs used among patients with polypharmacy infected with coronavirus also revealed benefits of using MRS-CDSS.5 Overall, we are glad to see a robust MRS-CDSS linked to the EHR, potentially reducing risks of ADE and improving patient safety.
However, after reviewing Ratigan et al.’s study, the study raises some important questions.2 This study reported the highest hazard ratios among patients aged 30-49 without providing further detailed information of their medication uses (e.g., total eras per person, days per era, days in study per person), which is critical for MRS calculations. Authors only listed this information between alive and deceased patients. Without such information, it is less clear why patients aged 30-49 might have higher risk of mortality with an increased MRS. Do these patients receive more acute episodic care and have fewer chronic disease conditions being managed? Do patients with short-term medications pose a higher risk of mortality in comparison to patients taking long-term medications? In addition, we understand patients’ mortality can be affected multi-factorially, and no study can analyze all potential confounders. However, some key confounders need to be included, such as Emergency Department visits, patient hospitalizations, or intensive care unit admissions, as well as did the death occur in the inpatient or out-of-hospital setting. Given the fact that more medications may be administered to patients who were admitted to hospitals or were under critical care conditions, it may correlate with higher MRS and higher mortalities. This association is remarkably interesting and will require further investigation.
References
(1) Raschke RA, Gollihare B, Wunderlich TA et al. A computer alert system to prevent injury from adverse drug events: development and evaluation in a community teaching hospital. JAMA 1998;280:1317-1320.
(2) Ratigan AR, Michaud V, Turgeon J et al. Longitudinal Association of a Medication Risk Score With Mortality Among Ambulatory Patients Acquired Through Electronic Health Record Data. J Patient Saf 2021;17:249-255.
(3) Bankes DL, Jin H, Finnel S et al. Association of a Novel Medication Risk Score with Adverse Drug Events and Other Pertinent Outcomes Among Participants of the Programs of All-Inclusive Care for the Elderly. Pharmacy (Basel) 2020;8.
(4) Bingham JM, Michaud V, Turgeon J, Axon DR. Effectiveness of an Advanced Clinical Decision Support System on Clinical Decision-Making Skills in a Call Center Medication Therapy Management Pharmacy Setting: A Pilot Study. Pharmacy (Basel) 2020;8.
(5) Al Rihani SB, Smith MK, Bikmetov R et al. Risk of Adverse Drug Events Following the Virtual Addition of COVID-19 Repurposed Drugs to Drug Regimens of Frail Older Adults with Polypharmacy. J Clin Med 2020;9.

This Post Has 0 Comments