Dermatology and podiatry in the Emergency Department? It can certainly happen. While not an emergency, definitely an interesting finding and affecting quality of life for the patient.
Case Report
60 yr. old male patient presented to the Emergency Department with a history of coronary arteriosclerosis, peripheral vascular disease, uncontrolled diabetes mellitus, hypertension, psoriasis, and history of intravenous drug abuse and alcoholism. The chief complaint was an unusual deformity of the toe-nails primarily affecting the great toes of both feet, and pain secondary to the overgrowth. The patient stated that he had a phobia of examining or touching his feet, and noticed that his nails had grown substantially in the past 5 years. He also stated that secondary to this phobia, he had refused to trim the toenails in approximately 9 years.
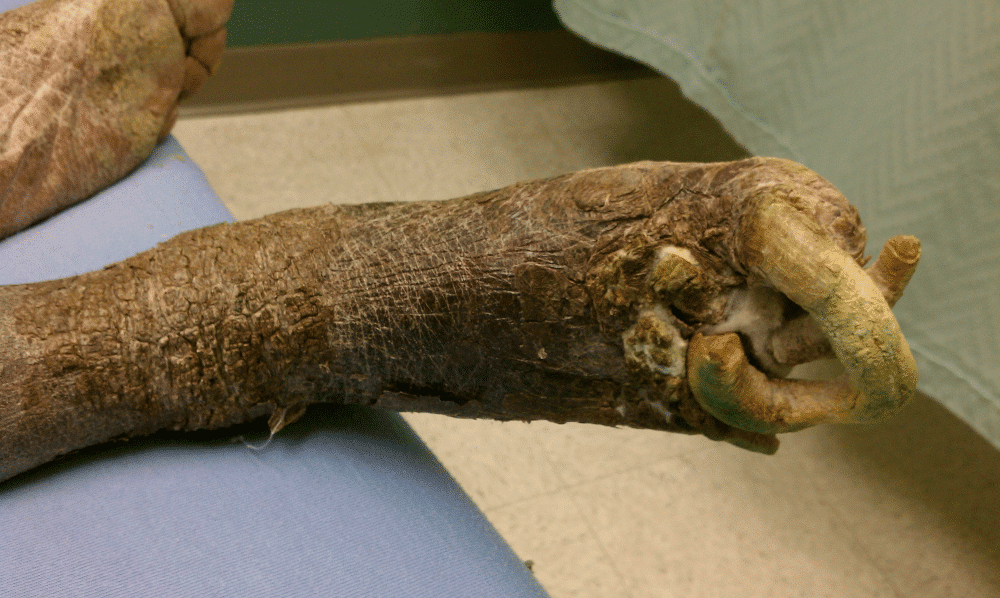
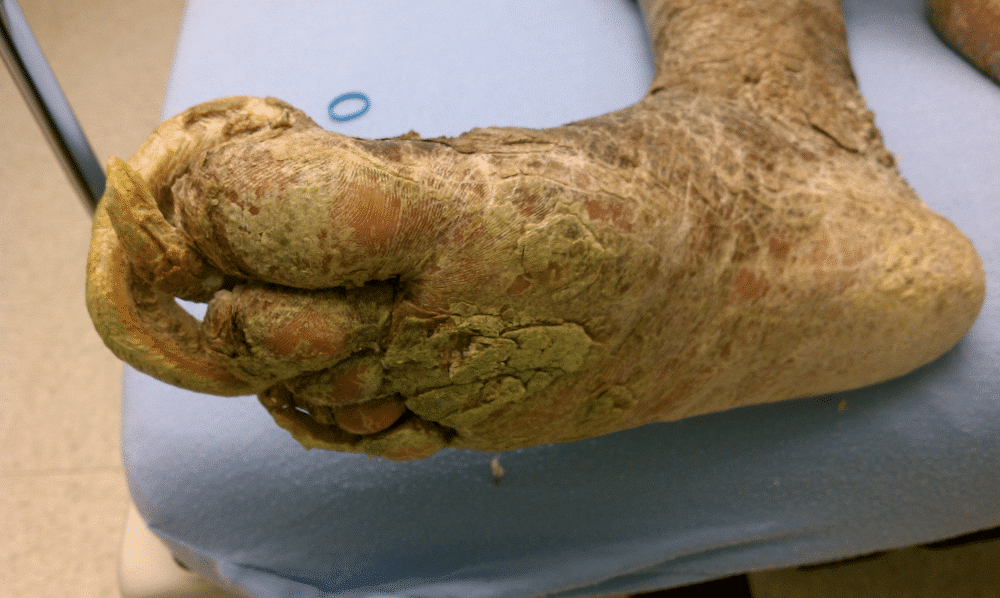
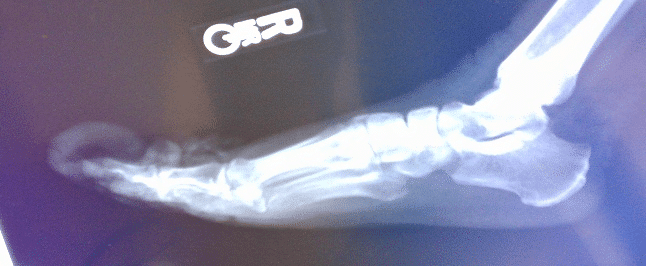
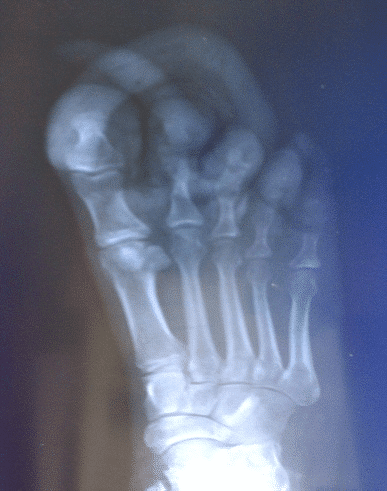
The nails had not been cut for a significant amount of time, with the resultant overgrowth noted at the time of the examination. There was presence of fulminant onychogryphosis of the toenails, as well as presence of stasis dermatitis, with resulting overlaying cutaneous hyperplasia, fissuring, and hemosiderosis (fig 1). The appearance of the skin of both lower extremities showed evidence of possible psoriatic lesions with positive Nikolsky sign and scaling appearance with skin sloughing. The presentation of the toenails showed evidence of underlying onychomycosis, with resulting hyperkeratosis of the nails. There was also evidence of psoriatic involvement of all extremity nails. The patient was noted to be non-compliant with diabetic medications, and had a history of long-standing peripheral neuropathy. Secondary to the deformity of his feet, underlying Charcot’s joint was also suspected with remodeling present. (fig 2)

(Fig.4). Lateral view. Plain film.
Discussion
Onychogryphosis is a severe deformation of the nail, most often affecting the great toes as the nail matrix is typically large enough to support the deformed nail. Onychogryphosis occurs when the nail plate thickens, the nail bed is hyperkeratotic, and uneven growth occurs at the matrix. The thick nail grows spirally, like a ‘ram’s horn’ leading to the name. Seen more commonly in the elderly but can occur in younger patients seen with onychomycosis or due to matrix injury or neglect. Grossly, the onychogryphotic nail will appear severely distorted, thickened, brownish, possibly spiraled, and unattached to the nail bed.
The nail plate is composed of 3 distinct layers: a dorsal thin layer, a thick intermediate layer, and a ventral layer4,5 . The healthy nail plate appears as a smooth, convex, nearly rectangular, translucent structure that has a pink color when light is reflected from its surface; the color is due to the underlying vascular-enriched nail bed. The nail matrix is the germinative portion of the nail complex, giving rise to the nail plate1,4,5. The matrix is at the most proximal point of the nail bed. Nail thickness is directly related to the length or the size of the nail matrix, thus, the nail matrix allows hypertrophy in cases of onychogryphosis.
To help in diagnosing or differentiating from mycotic nail dystrophies such as onychomycosis, biopsy of the nail plate and the hyponychium may be performed, such as and other dermatoses affecting the nail plate. Biopsy of the nail plate usually involves removing a piece of the distal plate along with a portion of the underlying hyponychium by using scissors, a bone rongeur, or a scalpel. (Not typically an ED procedure – Dermatology referral for outpatient management). At the target site, the punch is applied with moderate pressure against the nail plate, passing through the nail bed until it contacts the periosteum5,7,9. The punch is withdrawn, and the specimen is removed for histopathologic examination.
A technique that can be used to rule out onychomycosis is the noninvasive keratin biopsy. This biopsy technique has the added benefit of helping differentiate between hemosiderin versus melanic pigment in cases in which the nail has black or brown discoloration.
First-line treatment of onychogryphosis is to trim the deformed nails. If blood supply is satisfactory, urea ointment may be used to debride and avulse dystrophic nails in onychogryphosis, onychomycosis, and psoriasis, candidal and bacterial infections.
Complete excision of the viable nail matrix results in loss of the nail plate1,6,8. Therefore, a new nail plate cannot be regenerated.
Relative contraindications to performing surgery in the nail unit include the presence of established peripheral vascular disease, collagen vascular disease, diabetes mellitus, and disorders of hemostasis. Patients presenting with acute infection or inflammation of the nail unit, including the surrounding paronychial tissues, are considered to have relative contraindications to nail surgery. When possible, surgery in these patients should be postponed until the acute event has resolved3,5,10.
References
- Bywaters EG. Peripheral vascular obstruction in rheumatoid arthritis and its relationship to other vascular lesions. Ann Rheum Dis. 1957;16:84–103. [PubMed]
- Dawber RP, Baran R, Berker D. Science of the nail: gross anatomy. In: Baran R, Dawber RP, eds. Diseases of the Nails and their Management. Oxford, England: Blackwell Science; 1994:1-34.
- Dawber RP, Baran R. Diseases of the Nail. Oxford, England: Blackwell Science; 1994.
- Dawber RP, Baran R. Structure, embryology, comparative anatomy, and physiology of the nail. In: Baran R, Dawber RP, eds. Diseases of the Nails and their Management. Oxford, England: Blackwell Science; 1994:1-24.
- Haneke E. Surgical anatomy of the nail apparatus. Dermatol Clin. Jul 2006;24(3):291-6. [Medline].
- Kaplan JL and Porter RS, eds. The Merck manual of diagnosis and therapy (2011). Merck Sharp & Dohme Corp., A Subsidiary of Merck & Co., Inc., Whitehouse Station, NJ. Accessed 10/30/2011 via STAT!Ref Online Electronic Medical Library. http://online.statref.com/document.aspx?fxid=21&docid=384. 10/30/2011 7:08:41 PM CDT (UTC -05:00).
- Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, Loscalzo J. (2008). Harrison’s principles of internal medicine (17th ed.). New York: McGraw-Hill.
- Kechijian P. Onycholysis of the fingernails: evaluation and management. J Am Acad Dermatol. 1985;12:552–60. [PubMed]
- South DA, Farber EM. Urea ointment in the nonsurgical avulsion of nail dystrophies–a reappraisal. Cutis. Jun 1980;25(6):609-12
- White MI, Clayton YM. The treatment of fungus and yeast infections of nails by the method of “chemical removal’. Clin Exp Dermatol. May 1982;7(3):273-6.
- Winston JA and Miller JL, Treatment of onychomycosis in diabetic patients. Clin Diab. October 2006; 24(4):160-166.
- Wolff K, Johnson RA, eds. 2009. Fitzpatrick’s Color Atlas and Synopsis of Clinical Dermatology. New York. The McGraw-Hill Companies. ISBN 0-07-159975-4, ISBN 978-0-07-159975-7. STAT!Ref Online Electronic Medical Library. http://online.statref.com/document.aspx?fxid=14&docid=977. 11/6/2011 5:51:45 PM CST (UTC -06:00).
- Zaias N, Baden HP. Nails. In: Fitzpatrick TB, et al., eds. Dermatology in general medicine. 2nd ed. New York: McGraw-Hill, 1979;418–37.
- Zisova L, Valtchev V, Sotiriou E, Gospodinov D, Mateev G. Onychomycosis in patients with psoriasis – a multicentre study. Mycoses. 2011 Jul 20. doi: 10.1111/j.1439-0507.2011.02053.x. [Epub ahead of print]. Accessed 11/6/2011.
- Licciardone JC, Fulda KG, Stoll ST, Gamber RG, Cage AC: Osteopathic palpatory findings in type 2 diabetes mellitus: a case-control study .J Am Osteopath Assoc 2005, 105:320
Correspondence
Bradley Stoker DO FACFP.
Clinical Faculty – University of Utah Family Medicine. Wright Center for Graduate Medical Education, Department of Family Practice, Portland, Oregon.
Stefan Meyering DO FAAEM.
Associate Professor of Emergency Medicine – TCU/UNTHSC School of Medicine

This Post Has 0 Comments